By Vanessa Pratley
Investigative Journalist | Kaipūrongo Whakatewhatewha
Need to know:
Consumers are routinely paying thousands of dollars for hearing aids amid concerns that their welfare isn’t the top priority for clinics.
Large multinational manufacturers and retailers own more than 80% of hearing clinics in New Zealand, and just eight manufacturers control 90% of the hearing aid market worldwide.
Bundling and other pricing practices make it difficult for consumers to figure out what is included in the price of hearing aids and how much they really cost before engaging a clinic.
Some consumers report feeling unable to choose their own audiologist when making a claim to their insurer for lost or broken hearing aids.
It’s difficult for the average consumer to determine whether audiologists employed by multinational retail clinics are receiving commission or sales incentives or not.
Audiology as a medical profession remains unregulated by the government, exposing both audiologists and consumers to undesirable outcomes driven by the corporate nature of hearing care.
The Australian Competition and Consumer Commission put the hearing aid industry on notice in 2017 after similar reports emerged from consumers and clinicians, and we're calling on the Commerce Commission to do the same.
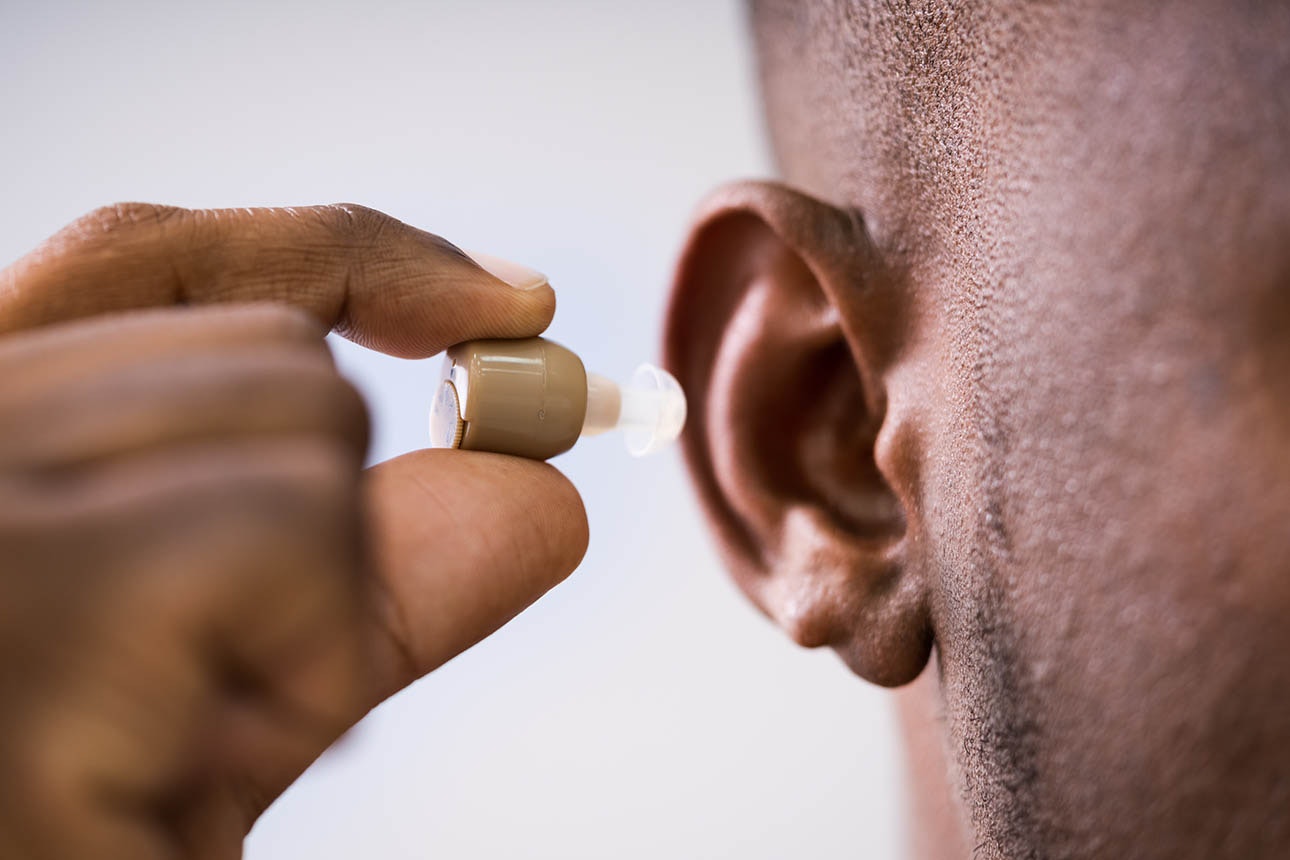
One in six people in New Zealand have some form of hearing loss. Even if you’re not one of them, you might have seen the ads or heard about the deals.
Claims like free hearing checks, aids from just $1 a day or even 10-day no-obligation trials may make you think it’s easy to get hearing aids.
If it’s so easy, why are only 17% of people worldwide who would benefit from hearing aids actually using them? It turns out that hearing loss comes at a cost, and it’s the biggest deterrent for New Zealanders.
With a government subsidy of only $511.11 per aid once every six years, those who are hard of hearing can end up paying thousands of dollars for aids.
We’ve heard from consumers and audiologists alike who are concerned there’s something amiss in the industry.
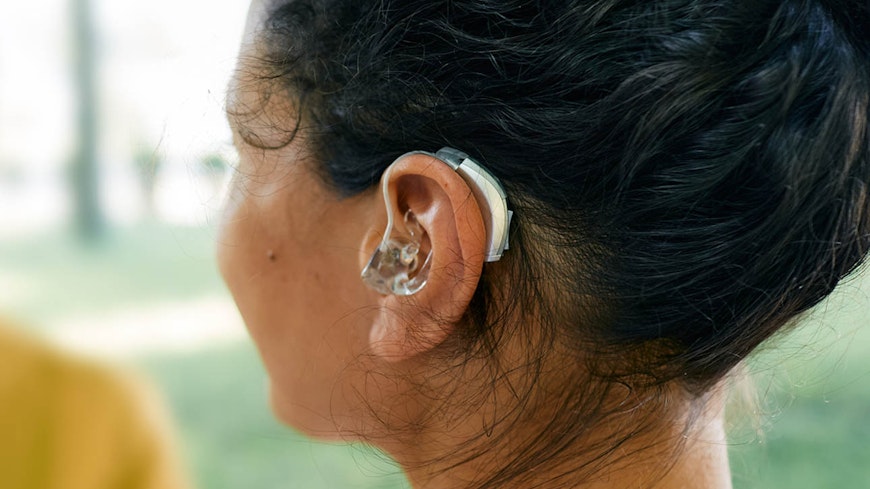
Stories from consumers
It took Dave* six years to pluck up the courage to get help with his hearing. He saw a Triton ad for its hearing aid guide and called the freephone number to get a copy. Triton booked Dave in for a hearing test at a clinic three hours away from where he lived. Dave decided to go along, just to see what could be done.
After driving to the appointment, Dave was rushed into a room and the testing began. He was given hearing aids and they were fitted.
However, Dave struggled with them. He has idiopathic sensory motor peripheral neuropathy. This makes it difficult to do things with his hands, including inserting fiddly devices into his ears.
He told the hearing professional this, and she said it would take practice to get it right. Dave said the hearing professional seemed like she was under time pressure. She removed the ‘wings’ of the aids, which are designed to hold them in place, because she decided he didn’t need them.
She told Dave he had a 10-day free trial of the aids to decide whether he wanted to buy them.
“The aids were fantastic – my car made noises I have never heard!”
However, they fell out twice during the drive back and they continued to fall out when Dave got home. All up, they fell out 15 times over 10 days. After a walk on the beach, he discovered one was missing.
While he was stressing about losing one of the aids, Dave got a call from Triton. The representative told him the trial was over and Triton needed his bank account details to deduct what he owed.
Dave was shocked.
Wasn’t it a free trial? He asked if they could discuss the issue, and after he told Triton he had lost one, he was told he’d signed a contract that committed him to a fee of $10,000. He would have to pay it.
“The whole appointment was compromised.”
He was never given a copy of this contract and wasn’t told about the conditions it contained. No one at the clinic explained to him that the aids cost $10,000 and that he would be liable to cover their cost if he lost one.
Dave contacted Consumer NZ’s advice line. After our advisers helped him fight back against the charge, he went to another clinic at which he got a similar pair of aids properly fitted for $6500 less than what Triton was charging.
A spokesperson for Triton said: “All of our clinicians follow best practice guidelines as laid out by [New Zealand Audiological Society]. Any responsibilities arising out of a trial period would have been made clear to Dave during the appointment. We are confident that customer complaints would have been handled to the highest standards and ultimately to the customer’s satisfaction.”
In a subsequent comment, Triton said it took Dave’s concerns seriously and resolved the complaint to his satisfaction.
But for audiologists and audiometrists alike, stories such as Dave’s are all too common. One audiologist told us they were “depressed but not surprised” to learn about his experience.
For other consumers, Dave’s story hits close to home. Mary* was prescribed hearing aids that were so ill-fitting, they hurt to wear. She had to take pain medication just to be able to use them.
Bill* couldn’t afford to buy new hearing aids but had a pair of aids that belonged to his late mother. He tried to get them refitted to meet his own hearing needs and arranged for a clinic to do this. But Bay Audiology, the clinic that originally dispensed the aids, complained and forced the other clinic to stop.
Bill described Bay Audiology’s actions as bullying.
Dean Lawrie, managing director at Bay Audiology, said in response to Bill’s experience: “We take very seriously any experience where we have not delivered to the ultimate satisfaction of every customer. I am distressed to learn of this highly unusual situation and would like the opportunity to connect with Bill to make things right.”
Bill finally got his aids sorted with cover from ACC.
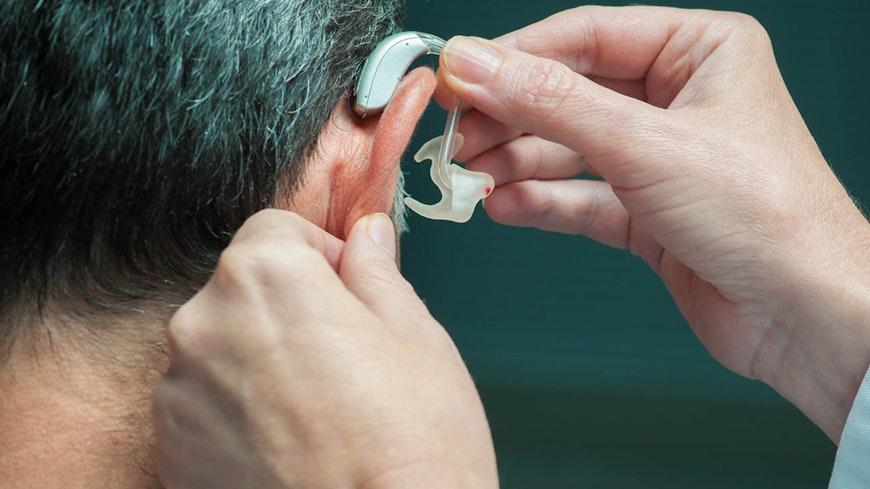
Overseas action
On the back of similar issues across the Tasman, the Australian Competition and Consumer Commission (ACCC) investigated clinicians’ and consumers’ concerns with the hearing aid industry. The ACCC put the industry on notice in 2017, calling for clinics to review their incentive programmes that had “the potential to cause widespread consumer detriment”.
In 2018, the ACCC started proceedings against Oticon and Sonic – hearing aid brands owned by manufacturer Demant. The ACCC alleged the brands misled consumers through advertising that targeted pensioners. They were found guilty and later fined $2.5 million.
As part of the 2017 investigation, some clinicians revealed they believed their employers were more focused on sales than independent advice, and some devices were recommended based on commission rather than consumer need.
In addition, some said failure to meet sales targets could result in termination of employment. When it came to price, some clinicians also felt worried about older consumers remortgaging their homes to pay for aids because of the high cost.
Consumers surveyed in Australia said they felt pressured into buying hearing aids that were more expensive. They felt clinicians were more interested in selling hearing aids than providing independent healthcare advice.
The consumers and clinicians we spoke to in New Zealand echoed these concerns.
The illusion of choice
In New Zealand, the big retailers – such as Triton, Audika and Bloom – are all owned by the manufacturers. The exceptions are Bay Audiology and Dilworth Hearing, which are both owned by Amplifon. Amplifon has its hearing aids manufactured through private-label agreements with other manufacturers.
Nevertheless, these large companies, manufacturer or not, own more than 80% of clinics in New Zealand. When the manufacturers of a product control other parts of the supply chain, such as the retailer, it’s called vertical integration.
There are far fewer independent clinics in New Zealand compared with vertically integrated clinics. Typically, an independent clinic is owned by the audiologist who runs it. These clinics are businesses too, but they’re often not subject to the same top-down commercial pressures that vertically integrated clinics are.
The ABC podcast that kickstarted the investigation in Australia revealed a clinic owned by manufacturer Sonova was offering audiologists a paid trip to a conference in Las Vegas to whoever sold the most aids. Sonova tracked the number of hearing aids sold using a medal tally, but this incentive wasn’t disclosed to consumers.
Commissions and sales incentives
We went to the major corporate hearing aid clinics operating in New Zealand and asked them if audiologists receive commissions or sales incentives to recommend certain brands.
Audika said: “[The company] is committed to providing excellent clinical care to its patients and makes recommendations based on a patient’s individual needs. Audika clinicians are free to recommend and order hearing aids from any manufacturer.”
Bay Audiology (owned by Amplifon) said: “While we do not pay commissions, employees are rewarded for meeting targets set for each clinic, spanning customer satisfaction, case audits, and business performance.”
Bloom told us: “We don’t have hearing aid-based commissions or sales incentives.” However, it has a “reward programme” that staff “can participate in”. The reward programme is based on performance of clinics measured against its business goals, and “one of the main qualifiers is behavioural alignment with WSA [WS Audiology] values and customer satisfaction”.
Dilworth (also owned by Amplifon) said: “Dilworth Hearing team members are in no way incentivised to choose one type of hearing aid over another. We do reward our employees for meeting specific clinic targets.” It explained that whether clinic targets are met depends on customer satisfaction, revenue, case audits and “Dilworth Hearing values”.
Triton said: "The compensation of our employees is aligned with Sonova Group's values, which is one of the four principles of Sonova's compensation policy. Sonova does not disclose further details of their compensation policy at the national or divisional level”.
Costs and fee bundling

We also asked most of the main clinics about bundled fees and services. Bundling is when the costs associated with getting hearing aids are merged with the cost of the aids, into a single price. This can include the cost of fittings, failed fitting fees (when a patient decides the aids aren’t right for them), getting moulds made, repair and ongoing maintenance costs, and batteries.
Bundling is a common practice in the hearing aid industry, but it means it’s hard for consumers to know how much they’re really paying for services.
These extra fees could add up to an estimated $1400 on top of the cost of two hearing aids, according to an ACC price list. But none of the clinics we asked would give us comprehensive information. Bay Audiology said it “does not add additional fees to the cost of the aid. Most aftercare services are provided at no charge to the client”.
Knowing how much you’re paying in extra fees is important given the government will only either subsidise $511.11 per aid (Hearing Aid Subsidy Scheme), or (if you meet the eligibility criteria) fund the cost of the aid (Hearing Aid Funding Scheme). The government won’t cover any of the other costs and it’s likely you’ll have to cover the shortfall, which could be hundreds or even thousands of dollars.
Dave’s experience also shows some clinics aren’t letting consumers know the estimated cost of the aids they’re trialling.
“If I had known they were that expensive, I never would have done the trial,” Dave said, describing it as “a misleading lack of information”.
This is why we think information on all fees associated with getting aids should be transparent, and the law agrees.
When it comes to the practice of fee and service bundling, Vanessa Horne, general manager of fair trading at the Commerce Commission, said misleading consumers about the price of a good or service is a breach of the Fair Trading Act.
“While businesses are free to set their own prices, any representations that a business makes about price must be clear, accurate and unambiguous,” she said.
“Businesses should not use fine print to hide additional costs or charges associated with a purchase.”
Horne also noted the Commerce Commission “is not currently investigating or looking into the retail hearing aid industry”.
Insurance woes
Some consumers insured with AMI, State, Westpac, BNZ, Co-operative Bank and ASB told us they have found it difficult to get replacement hearing aids through their own audiologist, because Triton has an agreement with IAG (Insurance Australia Group). The insurance group owns State and AMI and provides general insurance products (including contents insurance) for the other insurers listed.
Roy* told us that when he lost his hearing aid, he made a claim with his insurer. First, he said he dealt with his broker, who sent the claim to IAG to verify it. He’d given IAG a quote from his own audiologist to have them replaced, but IAG took a few days to get back to him.
According to Roy, the person on the phone asked him why he didn’t just use a provider like Triton. Roy said the person told him that he ought to admit he “threw them away” because “we deal with too many of these claims”.
The person on the phone, who Roy thought was from IAG, was “an assessor with Triton on behalf of IAG”, but they didn’t tell him until he asked.
Roy said he felt he was being pressured to use Triton after the assessor told him: “If you’re prepared to move to Triton, this’ll be an easier process.”
Despite insisting that he use his own audiologist, he said the person on the phone got angry.
Roy said they hung up when he expressed concerns that he was being manipulated. After speaking with his broker again, he finally got the hearing aids replaced through his preferred audiologist.
“I can imagine there’d be a lot of people that don’t know that you don’t have to give in to it, that you can go to your own audiologist, even though whoever it is makes it hard to.”
Colleen* shared her experience with us too, and her correspondence during the claims process echoes Roy’s troubles. An initial email sent to Colleen by Triton's insurance response team stated that claimants have two options.
The first option is a cash settlement. The letter qualifies the settlement by explaining that the cash might not cover the cost of replacement aids, as the claimant’s audiologist has “chosen not to be part of IAG’s hearing supplier programme”.
The second option is to go to Triton, which will cover up to $500 of the claim’s excess. The letter goes on to explain Triton’s promotions running at the time and emphasises its free hearing checks.
“The process was confusing, I felt like I was being railroaded,” Colleen said.
When we asked IAG about how the process worked, a spokesperson told us it engages a panel of hearing aid suppliers to replace broken or lost hearing aids. The suppliers on the panel are Sonova and Amplifon, with clinics Triton, Bay Audiology and Dilworth Hearing (see our table).
IAG confirmed that there were no independent audiologists or clinics currently on the panel.
The spokesperson said “having a panel in place allows us to keep prices fair for our customers. All audiologists are given the opportunity to work with IAG using our supplier process.” IAG said its priority is to keep insurance affordable and available.
“Consumers are given the choice to choose from our panel or a cash settlement with their own audiologist,” IAG said.
Even though Colleen was contacted by Triton in the first instance, IAG said “Colleen was given the choice to continue with her current audiologist first and foremost, then was given the option to use Triton if she wished.”
The Commerce Commission fined IAG $127,000 in 2006 after it pleaded guilty to 30 breaches of the Fair Trading Act. An IAG-owned insurer, State, misled customers about their right to choose their preferred windscreen repairer when it told them they had to use Smith & Smith, IAG’s preferred supplier at the time.
An unregulated profession
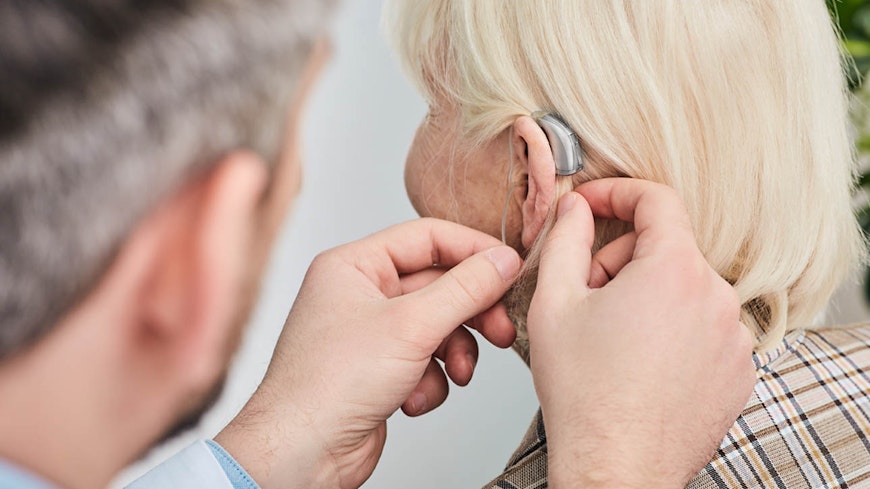
Audiology as a profession isn’t government regulated and anyone can call themselves an audiologist. Unlike doctors, nurses or chiropractors, audiologists aren’t legally considered health practitioners. We think they should be.
A spokesperson for the Ministry of Health said: “There are no plans in place to make audiology a registered health profession under the Healthcare Practitioner Competence Assurance Act.”
The spokesperson also said: “[It’s] not the only tool for ensuring competence and oversight of health professionals in New Zealand.”
Even though there isn’t any formal government regulation, the government does play an implicit role in regulating audiology. This is mostly in its role reducing costs for consumers by funding or subsidising hearing aids for people who meet the criteria.
Under the Hearing Aid Services Notice 2018, the subsidy or funding can only be used on specific, MOH-approved hearing aids. As at 10 February 2022, there were 15 brands of hearing aids on the approved devices list. Ultimately, out of 1724 hearing aids approved by MOH, more than 90% of them are from the big manufacturers.
The New Zealand Audiological Society (NZAS) is the self-regulatory body representing audiologists in Aotearoa. It prescribes standards of care that member audiologists must comply with, but membership is voluntary and there is scope for the ethics code to be more comprehensive when compared with an equivalent code used by Independent Audiologists Australia. Its code was written in consultation with Paul Komesaroff, a Professor of Medicine at Monash University and director of the Centre for Ethics in Medicine and Society.
Among other things, NZAS members are only required to disclose real or perceived conflicts of interest relating to finance. There is no requirement to disclose any other conflict.
Additionally, there is no requirement to be transparent about all fees, nor to provide reasonable and accurate estimates of fees. There are also no provisions relating to gifting.
To enforce the code, NZAS operates a complaints mechanism which could see an individual audiologist struck from membership. Unfortunately, NZAS has no jurisdiction to impose industry-wide standards or to oversee clinics more generally.
President of NZAS (at the time of writing) Karen Allen is a sales director at Bay Audiology. Allen is no longer president.
We’re calling for change
The issues in the hearing industry have the potential to affect more than 880,000 New Zealanders with some form of hearing loss. To ensure consumers such as Dave receive care that is consistent, ethical and cost effective, we’re calling for the following actions.
Clinics to review their pricing practices and be transparent about sales incentives and commissions.
The Government to meaningfully consider more robust regulatory options to support and protect consumers and hearing professionals.
NZAS to review and continue to actively enforce its codes of ethics and conduct to protect professionals from industry pressures.
The Commerce Commission to put the industry on notice.
If you’re considering buying hearing aids or getting a hearing test, visit our website for our updated hearing aid buying guide.
New Zealand’s hearing aid market
The number of complaints
Over the past seven years, consumers have made six complaints in total to the Health and Disability Commissioner (HDC) about individual audiologists and audiometrists. Over the same time, consumers made 42 complaints in total about hearing service providers; that is, clinics more generally.
Fifteen of the complaints about clinics were about a district health board (DHB) provider, but the remaining 26 were about private providers, independent or otherwise. The HDC wasn't sure about the remaining complaint, as it lost touch with the consumer.
Though most complaints made to the HDC concerning hearing services were about private clinics or providers, the HDC refused to tell us how many of those were against corporate-owned clinics rather than independent clinics as collating this information would have a significant negative impact on its ability to carry out its other functions. Complaints varied greatly and included issues with access to funding, treatment delays or refusals to treat, discrimination, inappropriate treatment and unexpected treatment outcomes.
*Names have been changed to protect privacy.

Our guide to buying hearing aids
Hearing aids cost anywhere from a few hundred to thousands of dollars. Here’s what you need to know before you buy.