By Belinda Castles
Researcher | Kairangahau
“We spot the spots that you might not,” MoleMap’s website claims. But unhappy customers tell us that’s not always the case and say the skin-imaging company has missed spots they’ve had to seek treatment for elsewhere.
Last year, we helped a Consumer NZ member get a $1386 refund and an apology after the company missed a non-melanoma skin cancer.
Since then, we’ve had more complaints about the company’s service.
Another member told us she’d received a $400 refund from the company after it failed to diagnose a basal cell carcinoma (a type of non-melanoma skin cancer).
With a history of melanoma, the woman had been getting annual check-ups at MoleMap for about 16 years, forking out approximately $7000 in fees.
MoleMap melanographers (registered nurses trained in skin cancer detection) use a dermatoscope to take magnified images of skin lesions. The images are sent to a dermatologist for diagnosis and treatment advice.
Concerned about a lesion on her forehead, the woman visited a dermatologist who referred her to a plastic surgeon to get it removed. A pathology report confirmed it was a basal cell carcinoma. The lesion had been identified by MoleMap earlier in the year, but its report didn’t state any action was required.
The woman contacted MoleMap to advise it of the missed lesion. MoleMap said it would investigate but didn’t get back to her. After three follow-up messages, her call was returned and she asked for a refund and an apology.
She was eventually given a refund and a free scan. The woman said she feels let-down by MoleMap, a company she’d relied on for many years.
“Despite my history of melanoma, MoleMap treated my misdiagnosed basal cell carcinoma like a broken toaster,” she said.
“The follow-up to my complaint was poor and the whole experience for a refund was a battle.”
A Napier couple also told us they were unhappy with the company’s complaints procedure. They asked MoleMap to examine two moles of concern, but only one was assessed. The couple didn’t discover this until the dermatologist’s report was emailed to them. When they complained, MoleMap thanked them for their feedback and said it “will be submitted for an internal inquiry”. The couple said the absence of a written record about their request to have both spots checked made it impossible to prove the checks done were not the checks asked for.
Last year, MoleMap told us the company was reviewing its complaints process.
Executive chair Jodi Mitchell said the company had since made improvements. “Notifiable events and complaints are now received and managed by a dedicated clinical excellence lead to ensure complaints are handled in a timely, thorough and empathetic manner.” Mitchell said the complaints we received pre-dated these changes but it would contact both customers.
Early detection
New Zealand Dermatological Society president Dr Louise Reiche said finding skin cancer as early as possible is key to successful treatment.
“The data shows that accuracy in diagnosing skin cancers and invasive melanomas is highest by a dermatologist in-person. However, in New Zealand we have a shortage of dermatologists [to meet] patient demand, which can lead to long waiting lists for an appointment. Seeing other doctors with extra training in skin cancer is the next best option,” she said.
Australia and New Zealand clinical guidelines state diagnosis of melanoma may be improved by clinicians trained in dermoscopy.
A 2020 review by the Cochrane Institute (an international organisation that systematically reviews health-care interventions) found that, when used by specialists, dermoscopy is better at diagnosing melanoma than visual inspection alone. The review concluded it may also help diagnose basal cell carcinomas.
Some skin clinics also offer skin checking or surveillance services. Cancer Society chief executive Lucy Elwood said it doesn’t endorse any commercial service but recognises mole mapping may be useful for some high-risk individuals to self-check.
“It is important that consumers are aware of variability in services and ask questions about the skin coverage checked, auditing of results, costs and follow-up,” Elwood said.
Before you make an appointment, check what services are offered and what they cost.
Self-checks important
Research suggests most skin cancers are first picked up through self-checks. A study of New Zealand patients diagnosed from 2012 to 2014 found 64 percent first noticed the abnormal lesions themselves, 16 percent were found by a family member and 14 percent by a doctor.
Health agencies recommend you do regular checks, including areas not normally exposed to the sun, such as the soles of the feet. Ask a family member or friend to check hard-to-see areas, such as your back, scalp and the back of your neck.
The ABCDEFG system is a good starting point for checking spots:
Asymmetry: one half is different from the other.
Border irregularity: the edges are poorly defined (uneven or blurry).
Colour is uneven: shades of brown, tan and black are present (other colours may also be present).
Different: it looks different from your other spots, freckles or moles (an “ugly duckling”).
Evolving: the spot has changed in growth (new, elevated or painful).
Firm: feels firm when you touch it.
Growing: most are larger than 6mm and keep growing.
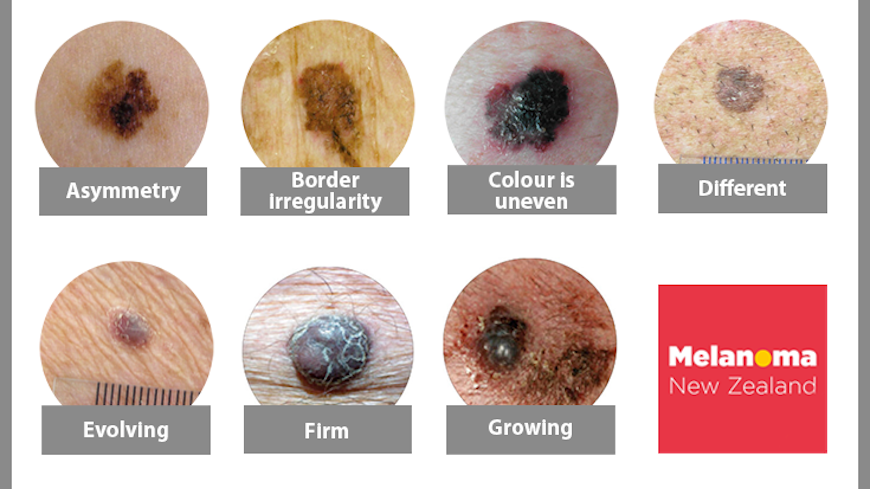
Images provided by Melanoma New Zealand. These images are indicative only. Look for the type of behaviour described, rather than trying to match your lesion to the images shown.
If your spot ticks any of these boxes – or even if you’re unsure – see your doctor or dermatologist.
By the numbers
Skin cancer is the most common cancer affecting New Zealanders. Melanoma is the most serious type of skin cancer, responsible for nearly 80 percent of skin cancer deaths. In 2018, 2738 people were diagnosed with it and 296 died of the disease.
Basal cell carcinoma (BCC) and squamous cell carcinoma (SCC) are more common than melanoma. Basal cell carcinomas are less dangerous than other forms of skin cancer and rarely spread. However, if left untreated, they can be serious.
Exact figures are unknown (new cases aren’t registered with the Ministry of Health’s Cancer Registry) but it’s estimated 80,000 people are treated for non-melanoma skin cancer each year.
Skin cancer apps
With a skin cancer app, you can use your smartphone to take a photo of a mole or lesion and get an assessment of its risk.
There are two main types of skin cancer apps:
Teledermatology or doctor report apps give you a risk classification based on the photo you send to a skin specialist.
Algorithm apps use a mathematical algorithm to analyse the photo and provide a risk classification.
Most apps will also require you to give a patient history, which includes your family history of skin cancer, the number of moles you have and whether your mole has changed appearance over time.
Are they accurate?
Dermatologist Dr Louise Reiche said apps aren’t yet reliable enough to replace in-person skin checks.
“The apps are good for encouraging people to check their skin and are useful for archiving images. However, a major concern is that consumers only take a photo of the moles they can easily see,” she said.
Dr Reiche also said it’s important the images are good quality, which requires a dermoscopic attachment for your phone and skills in using it.
Dermatologists are optimistic that as technology improves, the accuracy of these apps may also improve, she said.
Melanoma New Zealand said skin check apps can be useful for raising awareness and making people think about their skin, but they shouldn’t be relied on for diagnosis.
“There is still the potential for incorrect results which can give a false sense of security or create unnecessary anxiety. The technology is improving rapidly, so we are keeping an open mind – it’s a space to watch in the future,” said Melanoma New Zealand chief executive Andrea Newland.
A study published in 2020 in the British Medical Journal concluded that current algorithm-based apps weren’t reliable. The systematic review found accuracy studies assessing these apps were of poor quality. The studies only evaluated selected lesions and used images taken by experts rather than app users. Image quality was also noted as a major concern.
The Health Navigator Charitable Trust website, which independently reviews health apps, advises against using an automated algorithm app.
For its part, the Cancer Society doesn’t recommend smartphone apps to self-diagnose skin cancer.