We test the accuracy of blood pressure monitors.
One in five New Zealanders have high blood pressure (hypertension). If you’re one of them, you may find a home blood pressure monitor useful for tracking and managing your condition.
What to consider
Automatic or manual
Automatic monitors inflate the cuff automatically with the push of a button. Manual models require you to inflate the cuff by pumping a bulb. All the models we’ve tested are automatic monitors
Arm or wrist monitor

Monitors come with an arm or wrist cuff. Some arm models can be tricky to put on (as you’re doing it one-handed) but it’s easier to keep the cuff at heart-height for an accurate measurement. Following instructions on the cuff’s placement is important. Arm models typically have a larger, easier to read display, and are generally considered more accurate.
Using an app
Some monitors sync with an app, so you can track results.
Memory storage
Some monitors can store several blood pressure readings and some have separate memory storage for two or more users. This is a useful feature if you’re sharing the monitor with someone else in your household.
Display
The display should be big and clear, so it’s easy to read. The data should be easy to understand and stay on screen long enough to read.
Cuff size
It must fit snugly. Too tight will give you a higher reading, too loose may not give you one at all. Arm monitors generally come with a medium-sized cuff. If you’ve got large or small arms look for a brand that has different-sized cuffs available. Wrist monitors usually only come in one size.
Clinically validated
Check whether the monitor has passed international standard clinical tests. This information is usually found in the instruction manual or product packaging, and you can often find the information online.
Mains power adaptor
This can be handy if you run out of batteries. But you’ll need to purchase this accessory separately.
Irregular heartbeat display
This indicates when your heart rate isn’t steady. If you often get this warning, it’s a good idea to chat to your GP about it.
Hypertension or risk category indicator
This warning on the screen flags high readings and may be a good prompt to visit your GP. Some models have a traffic-light indicator scale on the side of the display so you can assess your risk.
Some blood pressure monitor arm cuffs are awkward to use to begin with, especially ones with a tube that runs to the monitor. But once you’ve used it a few times, you’ll sort out any ease-of-use issues.
What is blood pressure?
Blood pressure measures how hard your heart has to work to pump blood through the body. It’s measured as two numbers. The higher number (“systolic”) is the pressure in your arteries when your heart contracts or squeezes. The lower number (“diastolic”) is the pressure when your heart rests or relaxes between beats.
High blood pressure (hypertension) occurs when the force on your artery walls is higher than recommended. This can lead to damaged arteries and increase your risk of heart attack, stroke, heart failure and kidney and eye damage.
There’s no magic number that means your blood pressure is too high. In general, it’s considered elevated if it’s consistently more than 140/90 millimetres of mercury (mmHg). Your doctor may think you’re at risk even if only one of the two numbers is elevated. In weighing up your risk, you doctor will also consider factors such as your age, cholesterol levels, ethnicity, family history, weight and whether you’re a smoker.
Some people naturally have low blood pressure or hypotension (90/60 mmHg or lower), especially if they are very fit, which doesn’t cause any problems. But if you don’t naturally have low pressure and it gets low, you might start to feel dizzy and faint, which can be caused by an illness or injury. Some medications also lower your blood pressure.
An ideal adult blood pressure for most people is 120/80 mmHg or lower. It varies throughout the day and will be higher if you’re stressed, been exercising, eating salty food or consumed caffeine within a couple of hours of the reading . It also increases as you get older.
Why monitor?
High blood pressure is often called the “silent killer” because many people don’t know they have it. That’s why it’s important to be aware of your blood pressure according to Heart Foundation medical director and cardiologist Dr Gerry Devlin.
“High blood pressure usually doesn’t have symptoms but if left untreated can cause serious health problems such as heart disease, stroke, kidney failure and dementia. Managing high blood pressure is very effective in reducing the risk of a medical event and studies have found that home monitoring can help people keep their blood pressure under control,” Dr Devlin said.
A recent intervention published in 2021 in the British Medical Journal found that the management of hypertension by using self-monitored blood pressure led to better control of systolic blood pressure after one year than usual care.
Dr Devlin said home blood pressure monitoring is cost-effective, easy to incorporate in daily routines and lets you be more involved in managing your blood pressure.
“Monitoring can help you keep track of unexpected health changes and prompt you to see the doctor. This is particularly important when we’re dealing with the ongoing Covid pandemic and lockdowns. The downsides to home monitoring is it may lead to excessive monitoring and anxiety, or patients changing their treatment based on home measurements without consulting their GP,” he said.
Does the thought of visiting your doctor shoot your blood pressure up? You may have “white coat hypertension” – when your high reading is more due to nerves than an underlying medical condition. Monitoring your blood pressure at home when you are relaxed could give a more accurate result.
Monitoring can also be a good motivator if you’re trying to lower your blood pressure through lifestyle changes – is that kale smoothie and extra exercise class helping bring your pressure down.
Your doctor may recommend home monitoring to assess changes in your medication. It’s important you interpret blood pressure monitor results with your doctor.
Tips for using your monitor properly
When you first get your monitor, take it to your doctor to have its accuracy (and your technique) checked. Repeat this about every six months. Also get the monitor checked if you drop it or if readings change suddenly. Read the instruction manual to familiarise yourself with the monitor.
Take readings at the same time every day. Don’t smoke, drink caffeine, or exercise for at least 30 minutes before taking a reading. Morning measurements are best taken before breakfast and medications, evening readings should be taken after medications.
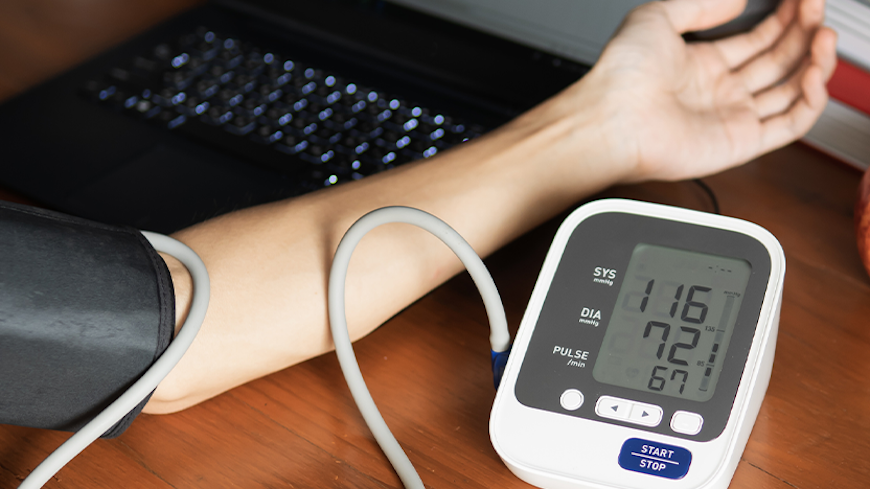
Sit on a sturdy chair with a supportive back, with your feet flat on the floor. Sit quietly for five minutes before you take your first reading. Your arm should be relaxed with the cuff at heart level.
Each time you take your blood pressure, take two consecutive readings (one minute apart). Don’t talk during this period. It’s useful to keep a diary.
Most manufacturers recommend getting your monitor serviced or calibrated every two years. This usually involves sending it back to the manufacturer, who may charge a fee.
Lifestyle tips for lowering your blood pressure
Quit smoking
Smoking causes your arteries to narrow (like high blood pressure does). If you have high blood pressure and smoke, you increase your risk of stroke.
Move it
Physical activity and maintaining a healthy weight are important to reduce your risk. Aim for 30 minutes of activity on most days of the week.
Limit alcohol
After a few drinks your blood pressure spikes. Regular heavy drinking can lead to long-term high blood pressure.
Eat less salt
Eating too much salt can increase your blood pressure. Many processed foods and takeaways are high salt options. On food labels, salt is listed as sodium. A low sodium option will have less than 120mg of sodium per 100g.



